Otosclerosis - Be Aware of Hearing Loss
Otosclerosis is a common disease among Caucasians, with studies indicating an incidence rate as high as 10% in this population, while the rate is lower among other ethnic groups. However, given the large population base in China, there are still many people affected by this condition, making it one of the important types of surgeries for experienced ear specialists.
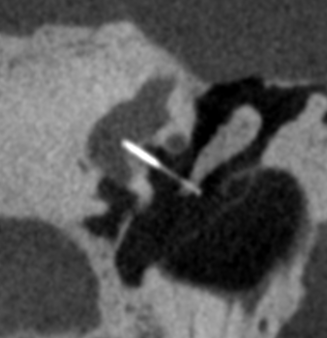
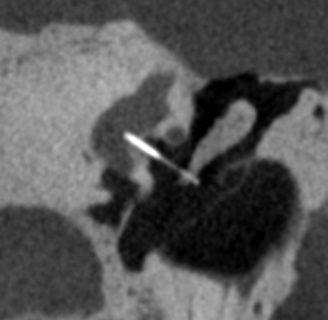
Otosclerosis, essentially refers to the condition where the stapes, the final ossicle responsible for transmitting sound in the middle ear, becomes immobilized due to pathological changes. It's akin to a chain (recommended term: ossicular chain) that should move and vibrate freely but becomes stuck due to rust, hindering effective sound transmission to the inner ear and leading to hearing loss.
Pathogenesis and Epidemiology
More common in Caucasians, predominantly in females, and typically affects those aged 30-50.
It may be partially related to genetics, but no specific pathogenic gene has been definitively identified.
Viral infections, endocrine disorders, and autoimmune factors may be potential risk factors.
Main Symptoms:
Most patients report a gradual decline in hearing. Since the initial stages of hearing loss are not easily perceived, the exact onset of the disease is often unknown. Patients may complain of a gradual decline in hearing over several years, which can be unilateral or bilateral. Some patients, due to a lack of attention to their hearing, might describe it as a "sudden hearing loss," although, in reality, it is just a sudden recognition, not the abrupt onset of the disease.
Some patients may experience tinnitus, which can be either low or high frequency. In fact, some patients may have a stronger desire for tinnitus treatment than for hearing improvement. In severe cases, it may even lead to vertigo or dizziness. Willis' paracusis: Poor hearing in normal environments but improved hearing ability in noisy environments. This is often not given much attention by clinicians and is therefore of limited significance.
Examination
Hearing Test: This is the initial and most crucial examination for identifying otosclerosis. An experienced audiologist is essential to accurately identify conductive hearing loss and assess its severity. This test demonstrates the hearing loss characteristics at different stages of otosclerosis.
CT Imaging: High-resolution CT scans can effectively identify otosclerosis. Beijing Friendship Hospital boasts the world's highest-resolution ear CT, with precision up to 50 microns, compared to the usual clinical CT precision of 300-700 microns. This provides a wealth of precise information about minute bone changes, especially for assessing ear conditions.
Treatment
Medication: There are currently only a few clinical reports on the use of medication to control the onset and progression of otosclerosis. For example, sodium fluoride and calcium supplements are believed to have some effect in alleviating the hearing loss and tinnitus associated with otosclerosis.
Hearing Aids: For patients who prefer not to undergo surgery, wearing hearing aids (HA) can be considered to improve hearing.
Surgical Treatment: Currently, stapedectomy with prosthesis implantation is widely recognized as the primary treatment method. It is important to note that surgery only improves hearing and does not halt disease progression. Whether the otosclerotic lesions progress rapidly or very slowly is unrelated to surgery. Surgery is a very delicate process. Since the stapes is immobile, doctors use a piston-like prosthesis, creating a small hole (approximately 0.6mm) in the stapes footplate using a drilling technique. One end of the prosthesis is attached to the incus, and the other end is inserted into the hole to transmit sound vibrations into the inner ear. The highest technology representing stapes prosthesis implantation today involves laser stapedotomy and laser perforation. The use of lasers greatly enhances the safety and efficiency of the surgery and is the most essential tool for surgeons performing this operation.
Risks
The surgical outcome carries certain risks. These include potential nerve damage, such as taste reduction and facial nerve dysfunction. Taste disturbances occur relatively more frequently but can generally be controlled within 5-10%, and it is believed that this sensory reduction can be slowly adapted to and compensated for. Facial nerve dysfunction, or facial paralysis, is extremely rare. To date, no irreversible permanent facial paralysis has occurred. The greatest surgical risk is hearing loss because the inner ear is considered open and faces some infection risk. If this occurs, the consequences can be severe, leading to irreversible sensorineural deafness. Severe postoperative dizziness may indicate an inner ear infection. The probability of this adverse event is extremely low, with the Friendship Hospital team having encountered no more than five such cases in over a decade of surgical experience.
Outcomes:
Successful surgical results can even eliminate the preoperative air-bone gap (ABG), meaning the air-conductive and bone-conductive hearing curves nearly overlap.
